Skin Longevity Starts at the Surface: Why Your Largest Metabolic Organ Sets the Pace for Whole-Body Aging
by Parallel Health Team
Skin is the body's largest organ, and the only one continuously interfacing with both the outside world and the internal environment. That dual position is not a passive accident of anatomy. The skin participates in vitamin D metabolism, xenobiotic detoxification (the breakdown and clearance of foreign chemicals), lipid handling, neuroendocrine signaling, and immune surveillance. When that surface organ becomes inflamed or dysbiotic (out of balance), the consequences do not stay at the surface. They travel inward, contributing to the chronic low-grade inflammation that drives biological aging.
True skin longevity is about supporting metabolic function and whole body health, not just aesthetic optimization.
Skin is a Metabolic and Immunological Organ, Not a Wrapper
For most of modern medical history, skin was treated as an envelope. The contemporary view is structurally different. The epidermis and its resident immune and microbial populations actively regulate human physiology.
Keratinocytes, the dominant cell type of the epidermis, the outermost layer of skin, secrete cytokines, chemokines, and antimicrobial peptides. Cytokines and chemokines are signaling molecules that immune cells use to communicate, and antimicrobial peptides are short proteins that kill or disable microbes on contact. Together, these signals shape both local and systemic immune tone, meaning they influence how inflamed or calm the rest of the body feels at any given moment. Keratinocytes also catalyze the first step of vitamin D production, converting a cholesterol precursor in the skin into vitamin D3 under UVB sunlight. Vitamin D in turn helps regulate barrier immunity throughout the body. Sebaceous (oil) and sweat glands contribute to lipid and cholesterol balance and help clear foreign chemicals, and reduced skin excretory capacity has been associated with elevated risk of metabolic syndrome, a cluster of cardiovascular and diabetes risk factors.
In other words, skin is doing biochemistry on your behalf around the clock. When that biochemistry is disrupted, the rest of the body notices.
Inflammaging: The Mechanism Linking Skin Health to Biological Age
The dominant theory of biological aging today centers on inflammaging, the chronic, low-grade, sterile inflammation that accumulates with age. "Sterile" here means the inflammation is not caused by an active infection. It is the body's immune system staying mildly switched on for years on end, and that quiet, persistent activation accelerates nearly every age-related disease, from cardiovascular disease and type 2 diabetes to neurodegeneration and certain cancers.
Skin contributes meaningfully to inflammaging in three ways.
First, skin is a major source of circulating inflammatory mediators. Severe inflammatory skin conditions such as psoriasis and atopic dermatitis (eczema) are now understood as systemic diseases, not just skin-deep problems. They raise levels of inflammatory signaling molecules in the bloodstream and have been linked in population studies to cardiovascular disease, metabolic syndrome, depression, and other comorbidities. Dermatology literature increasingly refers to this as the "inflammatory skin march," capturing the idea that inflammation starting in the skin can march outward into the rest of the body.
Second, age-related barrier impairment becomes a chronic inflammatory stimulus. As skin ages, transepidermal water loss (water evaporating out through the skin) rises and the barrier becomes leakier. A disrupted barrier itself induces local inflammation, and that inflammation feeds the same systemic pool that drives inflammaging.
Third, dysbiotic skin microbiota release pro-inflammatory antigens. When the microbial community on skin becomes imbalanced, bacterial components such as lipopolysaccharide (a piece of bacterial cell wall that the immune system reads as a threat signal) raise circulating levels of TNF-alpha, IL-1-beta, and IL-6. These are well-known inflammatory messengers. Chronic exposure to these signals contributes to cellular senescence (cells that have stopped dividing but refuse to die quietly), immunosenescence (an aging immune system that no longer responds well), and the senescence-associated secretory phenotype, or SASP, which is the cocktail of inflammatory molecules that senescent cells leak into surrounding tissue. All are hallmarks of biological aging.
This is not just mechanistic theory; it has been demonstrated in humans. A 2024 randomized study of 75 elderly women published in Clinical, Cosmetic and Investigational Dermatology found that applying a body moisturizer twice daily for four weeks significantly lowered serum levels of interleukin-6 (IL-6), one of the central inflammatory messengers in inflammaging, compared to untreated controls. Earlier work in aged mice produced the same pattern across a broader cytokine panel including TNF-alpha and IL-1-beta, and a current UCSF trial (the BIA Study) is extending these findings to a larger human cohort using widely available over-the-counter moisturizers. Restoring the skin barrier with a high-quality moisturizer (see: Blue Biotic™ or Skin Barrier Biotic™) is one of the simplest, most accessible interventions known to lower a measurable marker of systemic inflammation.
The clinical longevity field has begun to formalize this. Recent reviews of geroscience-informed dermatology highlight skin microbiome profiling, inflammatory signatures, and senescence markers as candidate biomarkers of biological age, alongside epigenetic clocks like Horvath, GrimAge, and PhenoAge. Epigenetic clocks estimate biological age (as opposed to chronological age) by reading chemical tags on DNA that change predictably over a lifetime.
The Skin Microbiome Builds and Defends the Barrier
The skin barrier is not built by keratinocytes alone. The microbiome is a structural co-author of the barrier itself.
Resident microbes regulate keratinocyte differentiation and stratum corneum formation (the way skin cells mature and stack into the tough outer layer of the barrier), modulate the protein seals between cells called tight junctions, and tune the chemical and immune gradients that keep pathogens out. For example, Staphylococcus epidermidis, a friendly commensal (a microbe that lives peacefully on us), produces antimicrobial peptides that crowd out genuinely harmful species like Staphylococcus aureus and Streptococcus pyogenes. Specific S. epidermidis strains release a molecule called lipoteichoic acid that calms one branch of the skin's inflammatory response, helping the skin distinguish friend from threat.
When your skin microbiome ecosystem becomes dysbiotic, the barrier degrades. Atopic dermatitis (eczema) is the clearest case study. Defects in filaggrin (a protein that helps hold skin cells together) and tight junctions co-occur with reduced microbial diversity, S. aureus overgrowth, and biofilm formation, in which bacteria build a protective slime layer that shields them from the immune system. The result is a self-reinforcing cycle of barrier loss and inflammation. Similar patterns appear in acne vulgaris, psoriasis, seborrheic dermatitis, and rosacea, leading several research groups to describe these conditions as "barrier organ" diseases that share mechanistic territory with inflammatory bowel disease, asthma, and celiac disease.
The implication for longevity is direct. A well-tended skin microbiome is not a luxury. It is part of the infrastructure that keeps systemic inflammatory tone low.
Why Microbiome Dermatology™ Belongs in a Longevity Protocol
Most longevity protocols today focus on the gut microbiome, sleep, exercise, fasting, and a handful of senolytic or senomorphic compounds. The skin remains underweighted, despite being the largest interface with the external environment and a quantifiable contributor to circulating inflammatory markers.
A skin-centered longevity strategy rests on four pillars.
- Measure the microbial state of the skin. Sequencing-based approaches such as whole-genome shotgun metagenomics read the full DNA of every microbe in a sample, rather than just identifying species. Adding absolute abundance quantification (counting how many of each microbe are actually present, not just their relative proportions) reveals not only who lives on your skin but what they are doing metabolically. This is the level of resolution required to act, rather than merely describe.
- Restore commensal function. Live and postbiotic interventions, targeted phage approaches that selectively reduce harmful bacteria, and barrier-supportive cosmeceuticals can shift dysbiotic communities toward configurations associated with low inflammatory tone.
- Protect the barrier. Lipid-replenishing formulations, gentle surfactants, and avoidance of barrier-disruptive ingredients reduce the chronic low-grade inflammation that fuels inflammaging.
- Track inflammation longitudinally. Skin microbiome composition, surface biomarkers, and emerging inflammatory signatures provide a non-invasive window into systemic aging trajectories, meaning we can watch how the body is aging without drawing blood or taking biopsies.
This is the framework Parallel Health calls Microbiome Dermatology™: treating skin as a metabolic and immunological organ whose microbial ecology can be measured, modified, and monitored as part of a broader longevity practice.
Frequently Asked Questions
Is skin really the largest organ in the body?
Yes. Skin covers the entire body surface, has a surface area of roughly 1.5 to 2 square meters in adults, and weighs more than any other single organ. Its size is one reason its inflammatory contribution to systemic biology is so significant.
What does it mean to call skin a "metabolic organ"?
Skin actively performs biochemistry on the body's behalf. It synthesizes vitamin D, breaks down foreign chemicals using a class of liver-style detox enzymes called cytochrome P450, regulates lipid and cholesterol balance through oil glands, neutralizes reactive oxygen species (the unstable molecules that damage cells), and excretes both internally produced and externally absorbed compounds through sweat. These functions feed into whole-body metabolic health, the same way the liver, gut, and kidneys do.
How does skin inflammation affect the rest of the body?
Inflamed skin releases inflammatory signaling molecules such as TNF-alpha, IL-17, IL-23, IL-6, and IL-1-beta into the bloodstream. Sustained release contributes to inflammaging, endothelial dysfunction (impaired functioning of the cells lining blood vessels, an early step toward heart disease), oxidative stress, and metabolic problems. Severe inflammatory skin diseases are associated with elevated risk of cardiovascular, metabolic, and psychiatric conditions.
What is the skin microbiome, and why does it matter for aging?
The skin microbiome is the community of bacteria, fungi, viruses, and archaea that live on and in the skin. It helps build the barrier, trains the immune system, and competes with pathogens. Dysbiosis is linked to increased inflammatory cytokine release, impaired barrier function, and accelerated aging.
What is the difference between skin barrier function and skin microbiome health?
They are tightly coupled but distinct. Barrier function refers to the structural and chemical integrity of the outer skin layer, including the flattened cells called corneocytes, the layered fats between them known as lipid lamellae, the protein seals between cells called tight junctions, and the slightly acidic pH on the skin's surface that discourages pathogens. Microbiome health refers to the diversity, composition, and metabolic activity of the resident microbial community. Each shapes the other. A disrupted barrier promotes dysbiosis, and dysbiosis degrades the barrier.
Can supporting the skin microbiome actually reduce systemic inflammation?
Mechanistic and translational evidence points in this direction. Restoring commensal organisms quiets inflammatory signaling at the receptors that immune cells use to detect microbes (Toll-like receptors), lowers local cytokine production, and re-establishes barrier integrity. Together these effects reduce a known contributor to the body's overall inflammatory load. Clinical endpoints linking these changes to validated longevity outcomes in humans are still emerging, and rigorous trials are ongoing.
How is skin longevity measured today?
Researchers and clinicians increasingly combine traditional dermatological assessments with epigenetic clocks (Horvath, GrimAge, PhenoAge), inflammatory signatures, senescence-associated markers, and skin microbiome profiling. AI-enabled platforms are being used to integrate these signals into composite biological age estimates.
What lifestyle factors most affect the skin microbiome?
UV exposure, air pollution, frequency and type of cleansing, antibiotic use, diet, sleep, stress, and the broader environmental microbial diversity around you all shape skin microbial communities. Modern indoor environments and reduced biodiversity exposure have been hypothesized to contribute to rising rates of inflammatory skin disease.
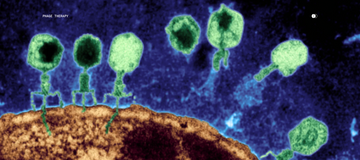
Where do bacteriophages fit into skin microbiome science?
Bacteriophages are nano-microbes that infect bacteria, and they are abundant on skin. They help regulate bacterial population structure and can be engineered to selectively reduce pathogenic strains while preserving commensals. In consumer contexts, this approach is sometimes referred to as phage therapy.
The Bottom Line
Skin is a metabolic organ, an immune organ, and an ecosystem. Its condition does not stop at the mirror. A compromised barrier and a dysbiotic microbiome contribute to the same chronic, low-grade inflammation that accelerates biological aging across every other system. Supporting the skin microbiome and its barrier is not separate from longevity work-- it is longevity work.
References
- Pilkington SM, Bulfone-Paus S, Griffiths CEM, Watson REB. Inflammaging and the Skin. J Invest Dermatol. 2021. Available at: https://pmc.ncbi.nlm.nih.gov/articles/PMC10669244/
- Chambers ES, Vukmanovic-Stejic M. Skin barrier immunity and ageing. Immunology. 2020. Related review on skin aging and immunosenescence: https://www.explorationpub.com/uploads/Article/A1003218/1003218.pdf
- Zhou H, Beltrán JF, Brito IL. The skin function: a factor of anti-metabolic syndrome. Diabetol Metab Syndr. 2012. Available at: https://pmc.ncbi.nlm.nih.gov/articles/PMC3567429/
- Yang Y, Qu L, Mijakovic I, Wei Y. Microbiome: Role in Inflammatory Skin Diseases. J Inflamm Res. 2024. Available at: https://pmc.ncbi.nlm.nih.gov/articles/PMC10876011/
- Yamanaka K. Special Issue: Skin Disease and Comorbidities. J Clin Med. 2021;10(24):5754. doi:10.3390/jcm10245754. Available at: https://pmc.ncbi.nlm.nih.gov/articles/PMC8707480/
- Sevilla A, et al. Skin, Autoimmunity and Inflammation: A Comprehensive Exploration through Scientific Research. Int J Mol Sci. 2023. Available at: https://pmc.ncbi.nlm.nih.gov/articles/PMC10650048/
- Bos JD, Kapsenberg ML. The Skin as an Immunologic Organ. In: Measuring Immunity. Elsevier. Available at: https://www.sciencedirect.com/science/article/abs/pii/S1571507805050014
- Nguyen AV, Soulika AM. Skin: a vast organ with immunological function. Exp Ther Med. 2019. Available at: https://pmc.ncbi.nlm.nih.gov/articles/PMC7271707/
- Szabó K, Erdei L, Bolla BS, Tax G, Bíró T, Kemény L. Are the Cutaneous Microbiota a Guardian of the Skin's Physical Barrier? The Intricate Relationship between Skin Microbes and Barrier Integrity. Int J Mol Sci. 2023. Available at: https://pmc.ncbi.nlm.nih.gov/articles/PMC10647730/
- Lee H-J, Kim M. Skin Barrier Function and the Microbiome. Int J Mol Sci. 2022;23(21):13071. Available at: https://pmc.ncbi.nlm.nih.gov/articles/PMC9654002/
- Prescott SL, et al. The skin microbiome: impact of modern environments on skin ecology, barrier integrity, and systemic immune programming. World Allergy Organ J. 2017. Available at: https://pmc.ncbi.nlm.nih.gov/articles/PMC5568566/
- Hong JY, et al. Microbiome-Based Interventions for Skin Aging and Barrier Function: A Comprehensive Review. Ann Dermatol. 2025;37(5):259-268. doi:10.5021/ad.25.009
- Marples R, Roberts D. Skin microbiome and host immunity: applications in regenerative cosmetics and transdermal drug delivery. Future Sci OA. 2018. Available at: https://pmc.ncbi.nlm.nih.gov/articles/PMC6060389/
- Albanesi C, et al. The Keratinocyte as a Crucial Cell in Atopic Dermatitis. Int J Mol Sci. 2021. Available at: https://pmc.ncbi.nlm.nih.gov/articles/PMC8509070/
- Chiricozzi A, et al. The Influence of Microbiome Dysbiosis and Bacterial Biofilms on Epidermal Barrier Function in Atopic Dermatitis. Int J Mol Sci. 2021. Available at: https://pmc.ncbi.nlm.nih.gov/articles/PMC8395079/
- Santoro A, Ostan R, Candela M, et al. Microbiomes other than the gut: inflammaging and age-related diseases. Semin Immunopathol. 2020. Available at: https://pmc.ncbi.nlm.nih.gov/articles/PMC7666274/
- Translating Geroscience Into Clinical Longevity Dermatology: From Mechanisms of Aging to Skin-Centered Interventions. J Cosmet Dermatol. 2025. Available at: https://pmc.ncbi.nlm.nih.gov/articles/PMC12729496/
- Inflammation-Driven Molecular Ageing in Chronic Inflammatory Skin Diseases. 2025. Available at: https://pmc.ncbi.nlm.nih.gov/articles/PMC12469205/
- Boismal F, et al. Cellular Senescence and Inflammaging in the Skin Microenvironment. Int J Mol Sci. 2021. Available at: https://pmc.ncbi.nlm.nih.gov/articles/PMC8068194/
- Li Z, Bai X, Peng T, et al. How Microbiomes Affect Skin Aging: The Updated Evidence and Current Perspectives. Life (Basel). 2022. PMID: 35888025. Available at: https://pubmed.ncbi.nlm.nih.gov/35888025/
- Inflammaging in human photoexposed skin: Early onset of senescence and imbalanced epidermal homeostasis across the decades. bioRxiv. 2022. Available at: https://www.biorxiv.org/content/10.1101/2022.03.28.486066.full.pdf
- Gut Microbiota, Probiotics, and Aging: Molecular Mechanisms and Implications for Healthy Aging. 2025. Available at: https://pmc.ncbi.nlm.nih.gov/articles/PMC12828327/
- Shimoda-Komatsu Y, et al. Correlations Between Serum Cytokine Levels and the Use of a Moisturizer in Elderly Women in Accordance with the Improvement of Objective and Subjective Skin Condition. Clinical, Cosmetic and Investigational Dermatology. 2024. Available at: https://pmc.ncbi.nlm.nih.gov/articles/PMC10829507/
- Ye L, et al. Topical applications of an emollient reduce circulating pro-inflammatory cytokine levels in chronically aged humans: a pilot clinical study. J Eur Acad Dermatol Venereol. 2019.